I am asked this all the time, “IBS vs IBD, what’s the difference?”
While people tend to use the terms interchangeably and they share many of the same symptoms, there are major differences between IBS (Irritable Bowel Syndrome) and IBD (Inflammatory Bowel Disease).
Warning: this post is lengthy and contains a ton of resources, references, and even more sources/links to check out. It’s because this post was first written in 2016. I then updated and republished it at the end of 2020.
During the past 4 years, I have not only done a ton more research, but I’ve also heard all the IBS and IBD stories. My father passed away from Colon Cancer. And finally, I myself, healed (SIBO; Colitis, suspected remission, a clean scope as of 2018).
So with all of that in mind…..
IBS vs IBD: What’s the Difference?
Click HERE to save IBS vs IBD for later.

The overarching difference between IBS vs IBD is that while IBS does not create structural changes in the gut, IBD does.
For years, I was told it was “just” IBS, and then I was diagnosed with Colitis.
You can read all about it via my story.
Know someone who might benefit from this information?
Click HERE to save it to your Pinterest, HERE to share it on Facebook or grab this link -> https://bit.ly/aggibsvsibd to email anyone!
This isn’t just accessory information. Knowing the difference between IBS vs IBD could be life-saving information.
What is IBS?
Click HERE to save this for later.

IBS stands for Irritable Bowel Syndrome. It is classified as a syndrome, not a disease.
Most people with IBS will never develop IBD, but most people with IBD have IBS symptoms, which is why I always say IBS and/or IBD.
IBS is known as “spastic colon,” and since it’s a syndrome it’s just a set or range of symptoms that may fall into the defining category, Irritable Bowel Syndrome.
IBS, unlike IBD, does not cause tissue inflammation. In other words, if you were to be ‘scoped,’ doctors would not find tissue inflammation, scarring, etc. from IBS alone. (However, if you were scoped and did have a form of IBD, you would discover that. It would not be a pleasant finding, but critical.)
Even though there is no permanent damage done with IBS, it still can cause day-to-day pain, discomfort and misery for those who battle it. This is why I never say “it’s just IBS.” And that’s also why I always put “just” in quotation marks.
I see your pain.
According to the International Foundation for Functional Gastrointestinal Disorders, IBS affects at least 10% to 20% of adults in the U.S. — mostly women — and is second only to the common cold as a cause of absenteeism from work. (source)
(And now you know why I’m so passionate about helping women in particular!)
Finally, and this is something that people overlook all the time, but for which I’ve set out to help with because it’s exactly what happened to me!
IBS usually begins in late adolescence or early adult life — most often at times of emotional stress. Source

Get off the hamster wheel today.
Reduce bloat and normalize weight by getting out of the start-and-stop “gut healing” cycle. In just 21 short days, you’ll be light years ahead of where you’re at today.
What are the Symptoms of IBS?
Everyone is different, namely because some have the IBS-C (constipation) version and others have the IBS-D (diarrhea) version while others have the alternating version which includes both constipation and diarrhea.
But in general, here are many of the IBS symptoms:
- abdominal pain
- constipation
- diarrhea
- both constipation and diarrhea, alternating
- gas
- bloating and/or distention (not the same things)
- mucus in stool
- nausea
Read more about IBS via What is IBS C and D.
And track those symptoms easily with my gut healing journaling SYSTEM.
Seriously, this journal was created specifically for those with IBS and/or IBD or those who have a haunch that’s what is likely going on. You can use it on your own or (better yet) in conjunction with your medical practitioner.
What Causes IBS?
To be clear, no one truly knows what causes IBS.
Here are some theories:
- Disturbance in the gut-brain axis.
- Irregular colon motility patterns. In other words, how fast food moves through you is either too fast or too slow.
- SIBO!!!
- Mild celiac disease that damages the intestines, causing IBS symptoms”
- Dysbiosis of the microbiome
Let me be very clear, I think the statement “it’s just IBS” is BS.
I believe that when given the diagnosis “IBS,” there is always more to the story. Said IBS doesn’t get any better, usually gets worse, because the root cause is not determined.
In fact, HERE are 7 roots causes of IBS.
Who Gets IBS?
In the United States, estimates of 10-15 percent of the adult population suffers from IBS symptoms.
- Women of reproductive age represent a significant portion of patients with irritable bowel syndrome (IBS).
- IBS affects about twice as many women as men, most often in people younger than 45 years.
- Studies suggest that about 5 percent of children ages 4 to 18 years old have IBS.
- A lot of teens have IBS, showing an estimate of between 6% and 14% of all teens have IBS symptoms. It seems to affect more girls than guys.
For more, check out 14 Irritable Bowel Syndrome Stats.
What Does IBS Poop Look Like?
This is a great question!
IBS poop is almost always a 1-2 and/or 6-7 on the Bristol Stool Scale.

Additionally, the color can be anything from very pale to tarry (ie very dark or black).
Keep in mind that anything bright red or black for an extended period of time is not good.
This indicates blood, and you definitely need to see a doctor.
What is IBD?
Click HERE to save this information for later.

IBD stands for Inflammatory Bowel Disease. It is classified as a disease, not a syndrome.
Unlike IBS, IBD causes changes in bowel tissue and increases your chances for colorectal cancer (source). Because of these changes, IBD is detectable via diagnostic imaging.
IBD involves chronic inflammation on all or part of the digestive tract, and it primarily includes ulcerative Colitis and Crohn’s disease. IBD affects about 1.6 million Americans, most of whom are diagnosed before age 30 (source).
There is no cure for IBD. However, the disease can go into remission.
What are the Symptoms of IBD?
Like everything else, symptoms are unique to the individual and the type of IBD present.
But here are some common symptoms seen in those with IBD:
- severe diarrhea
- pain
- fatigue
- weight loss
- bleeding and/or black stools
- night sweats
- loss of normal menstrual cycle
- loss of appetite
- additional: vomiting, anemia, fevers
What Causes IBD?
Similar to IBS, no one knows for sure what causes IBD.
We do know that it is known to involve an interaction between genes, the immune system, and environmental factors. I like to call the the not-so-perfect storm.
- Genetics are a clear factor. CCFA states, ” Studies have shown that 5% to 20% of affected individuals have a first-degree relative (parent, child, or sibling) with one of the diseases.”
- Environmental triggers like: smoking, antibiotics, NSAID’s, and diet.
- Weak immune system from any of the above environmental factors and/or anything else that creates a weakened immune system.
Who Gets IBD?
Did you know that most people are diagnosed with IBD before age 35?
- Approximately 1.6 million Americans currently have IBD, a growth of about 200,000 since the last time the CCFA (Crohn’s and Colitis Foundation) reported this figure (in 2011).
- As many as 70,000 new cases of IBD are diagnosed in the United States each year.
- There may be as many as 80,000 children in the United States with IBD.
- Has no gender preference (though some sources state men get it more than women).
- Is most common in Jewish individuals and those with origins in Northern Europe.
What are the Most Common Types of IBD?
While IBD is the umbrella category, there are specific diseases that fall within the category.
The two most common types of IBD are Crohn’s Disease and Ulcerative Colitis.
While they are frequently lumped together in discussion, they are not the same.
What is Crohn’s Disease?
Crohn’s Disease can affect any part of the GI tract, from mouth to anus. It can exist in “patches” vs. streamlined.
- It most commonly affects the end of the small intestine (the ileum).
- The inflammation may extend through the entire thickness of the bowel wall.
Crohn’s can be broken down further by type:
- ileocolitis
- ileitis
- gastroduodenal Crohn’s disease
- jejunoileitis
- Crohn’s colitis
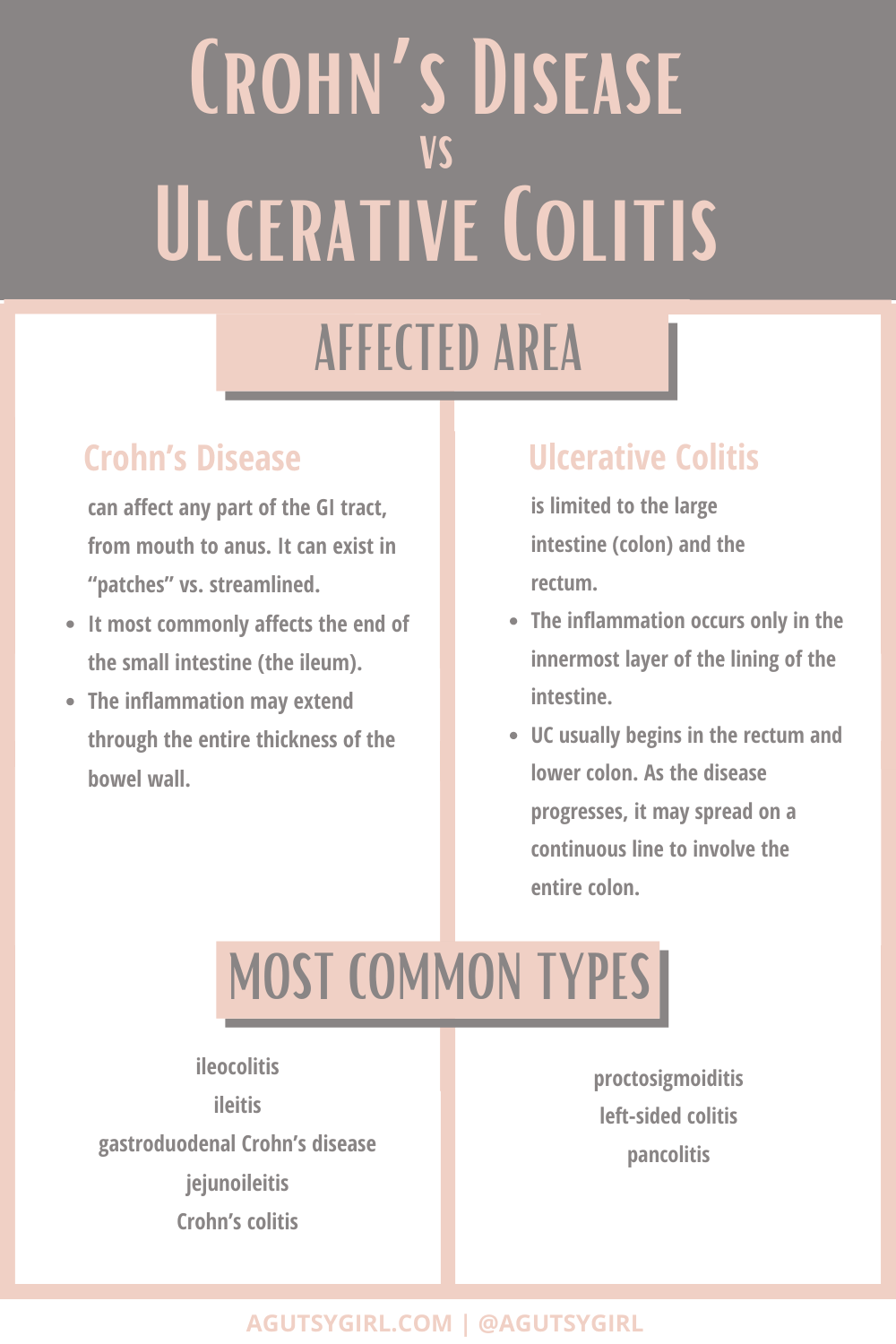
What is Ulcerative Colitis?
Unlike Crohn’s Disease, Ulcerative colitis is limited to the large intestine (colon) and the rectum.
- The inflammation occurs only in the innermost layer of the lining of the intestine.
- UC usually begins in the rectum and lower colon. As the disease progresses, it may spread on a continuous line to involve the entire colon.
Three common types of Ulcerative colitis include:
- proctosigmoiditis
- left-sided colitis
- pancolitis
By the way, there are many more beyond this. For example, I was diagnosed with Proctitis.
More sources: HERE, HERE, HERE, HERE, and HERE.
How Do I Know if I Have IBS or IBD?
Click HERE to save these steps for later.

Step 1:
Stop Googling. (Unless you’re using it in conjunction with my gut healing journaling SYSTEM to help gather information prior to step 2.
Step 2:
Find a great doctor, and if you can, seek out a Naturopathic/Holistic doctor (MD). Wondering how to find a Naturopathic/holistic doctor? Click HERE for How to Find an Integrative Medicine Doctor. If you choose a traditional western medicine doctor, seek out referrals prior to seeing him/her. Trust me, I spent far too long trying to find a good one.
Step 3:
Based on your physical, symptoms and more, your doctor will determine if you need a colonoscopy and/or endoscopy (I’ve had both) or other further testing like blood samples, stool samples, x-rays, etc. (I’ve done several) for final determination.
Step 4:
Based on Step 3, a final conclusion will be made. Having said that, without step 3, a final conclusion cannot be made because you cannot determine IBD without specific diagnostic tests.
I understand being scared, spending money on testing, and going through any and all of it. I’m here to listen and help however I can. I created The Beginner’s Guide to Digestive Health Testing to help get you started.
What are the Treatments for IBS and IBD?
Click HERE to save these treatment options for later.

This one is 110% subjective based on your doctor, personal beliefs, and choices.
Furthermore, the treatment can be dictated by the stage and severity of the IBS and/or IBD and even whether it’s IBS and/or Crohn’s Disease or Ulcerative colitis specifically.
Here is a list of several treatment options (not an exhaustive list and not including many/going into detail on lifestyle things which are huge factors):
- Dietary changes (both)
- more or less fiber
- increase water
- specific dietary changes and/or dietary protocol templates (that you then customize for you)
- avoid or cut caffeine and alcohol
- LDN (both)
- Antibiotics (IBD)
- ciprofloxacin
- metronidazole
- Stress management (both)
- Immunomodulators (IBD)
- azathioprine
- 6-mercaptopurine (6-MP)
- methotrexate
- Acupuncture (both)
- Anti-diarrhea medication (IBS)
- Antidepressant medications (both)
- Corticosteroids (IBD)
- prednisone
- prednisolone
- budesonide
- Aminosalicylates (IBD)
- sulfasalazine
- balsalazide
- mesalamine
- olsalazine
- Metronidazole (Flagyl) (IBD)
- Biologic therapies (IBD)
- Humira
- Remicade
- Cimzia
- Entyvio (Tina from Carrots ‘n Cake uses this. If you want to see more about her Colitis journey, check it out HERE.)
- Psychological therapy (both)
- Pain relievers (both)
- Surgery (IBD)
- Supplements (both)
I am passionate about gut health and in particular, women who have IBS and/or IBD.
Why?
Because IBS and IBD affects women mostly, and yet, most women are so embarrassed by it that they suffer, alone, in silence.
I don’t want this for you!
Keep exploring and seeking those answers, darling.
If you liked this post on IBS vs IBD you might also enjoy:
Xox,
SKH
🤰 bloating be gone! weight loss through optimal gut health for women
💃ʜᴇᴀʟ ʏᴏᴜʀ ɢᴜᴛ. ʜᴇᴀʟ ʏᴏᴜʀ ʟɪfe.
🫶🏻 founder gutbyome.com







I am totally the IBS queen over here.
Ugh.
Not sure if I am proud of it? lol
Ha. I’m not sure we ever have to be “proud” of it, but surely we should not feel shamed because of it! xo
Thank you! Yes, please do a blog post about how to find a good holistic MD! 🙂
Noted!