It seems like the questions around histamine intolerance are coming in more often than ever before.
So I wanted to spend the time researching and addressing any and all histamine intolerance information for you today.
Histamine (2-[4-imidazolyl]ethylamine) was discovered in 1910 by Dale and Laidlaw. It was identified as a mediator of anaphylactic reactions in 1932.
All of the below (unless otherwise noted/sourced) taken from the Chris Kresser ADAPT Academy Program I am part of.
What is Histamine?

Histamine is a natural chemical in our bodies that acts as a neurotransmitter. It is involved in muscle contraction, brain function, and the regulation of stomach acid. It also plays an important role in the immune system.
Histamine levels in the blood from 0.3 to 1.0 nanograms per milliliter are considered to be normal. Everyone has a threshold of histamine that they can tolerate without symptoms.
What Does a Histamine Intolerance Look Like?
When there is too much histamine, it can cause an allergic reaction with the following symptoms:
- Redness
- Swelling
- Itchiness
- Hives
- Red eyes
- Nasal congestion
- Runny nose
- Headache
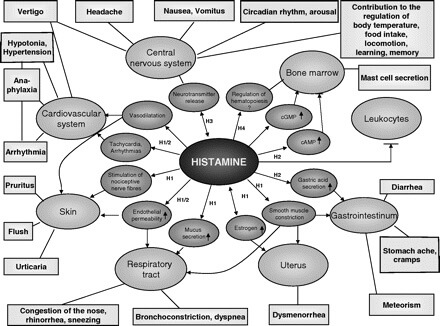
(Figure taken from HERE.)
Skin rashes can also be a sign of an allergic reaction known colloquially as “histamine intolerance.”
This typically refers to a defect in the body’s ability to break down histamine and/or a shift in the gut microbiota that leads to an increase in histamine-producing intestinal bacteria.
Dr. Amy Myers also points out these other signs/symptoms:
- Do you experience unexplained headaches or anxiety?
- What about irregular menstrual cycles?
- Does your face flush when you drink red wine?
- Do you get an itchy tongue or runny nose when you eat bananas, avocados, or eggplants?
If you answered yes to any of these questions, then you could have a histamine intolerance.
Note: Recent research suggests that what many patients and clinicians have referred to as histamine intolerance may be better characterized as mast cell activation syndrome (MCAS). MCAS is a condition involving hyperactivity of the mast cells that produce histamine. The etiology and pathology of MCAS are still poorly understood, and it is likely a heterogenous disorder with causes and expressions that vary among individuals.
DAO Enzyme
“Once formed, histamine is either stored or broken down by an enzyme.
Histamine in the central nervous system is broken down primarily by histamine N-methyltransferase (HMT), while histamine in the digestive tract is broken down primarily by diamine oxidase (DAO).
Though both enzymes play an important role in histamine break down, the American Society for Clinical Nutrition found that DAO is the main enzyme responsible for breaking down ingested histamine.
So if you’re deficient in DAO, you likely have symptoms of histamine intolerance.”
Amy Myers MD
Dr. Amy Myers lists the following as causes of low DAO:
- Gluten intolerance
- Leaky gut
- SIBO
- DAO-blocking foods: alcohol, energy drinks, and tea
- Genetic mutations (common in people of Asian-descent)
- Inflammation from Crohn’s, ulcerative colitis, and inflammatory bowel disease.
- Medications:
- Non-steroidal anti-inflammatory drugs (NSAIDs) (ibuprofen, aspirin)
- Antidepressants (Cymbalta, Effexor, Prozac, Zoloft)
- Immune modulators (Humira, Enbrel, Plaquenil)
- Antiarrhythmics (propanolol, metaprolol, Cardizem, Norvasc)
- Antihistamines (Allegra, Zyrtec, Benadryl)
- Histamine (H2) blockers (Tagamet, Pepcid, Zantac)
I share these because, just look – it’s all tied to the gut.
How to Test for Histamine Intolerance
Histamine intolerance is unlike other food allergies or sensitivities in that the response is cumulative, not immediate.
The example Chris Kresser gives is this: Imagine it like a cup of water. When the cup is very full (high amounts of histamine in the diet), even a drop of additional water will cause the cup to overflow (symptoms activated). But when the cup is less full, it would take more water (histamine) to cause a response. This makes histamine intolerance tricky to recognize.
Furthermore, there aren’t any reliable lab tests for accurately diagnosing MCAS or histamine intolerance because many people with MCAS have normal serum histamine and DAO levels.
So, how to diagnose it?
If you have a skin condition, consider that histamine intolerance might be the underlying cause—especially if you have one or more of the allergy-related symptoms mentioned above. In these cases, a low-histamine diet can be started to bring histamine levels down and hopefully clear up his or her skin.
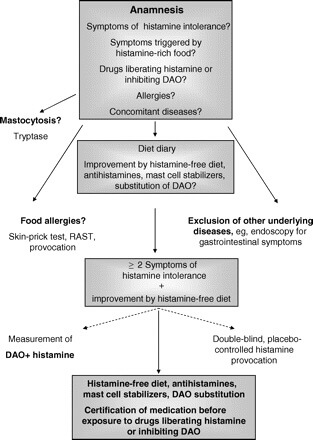
(Figure taken from HERE.)
Low Histamine Diet
Click HERE to save this for later.
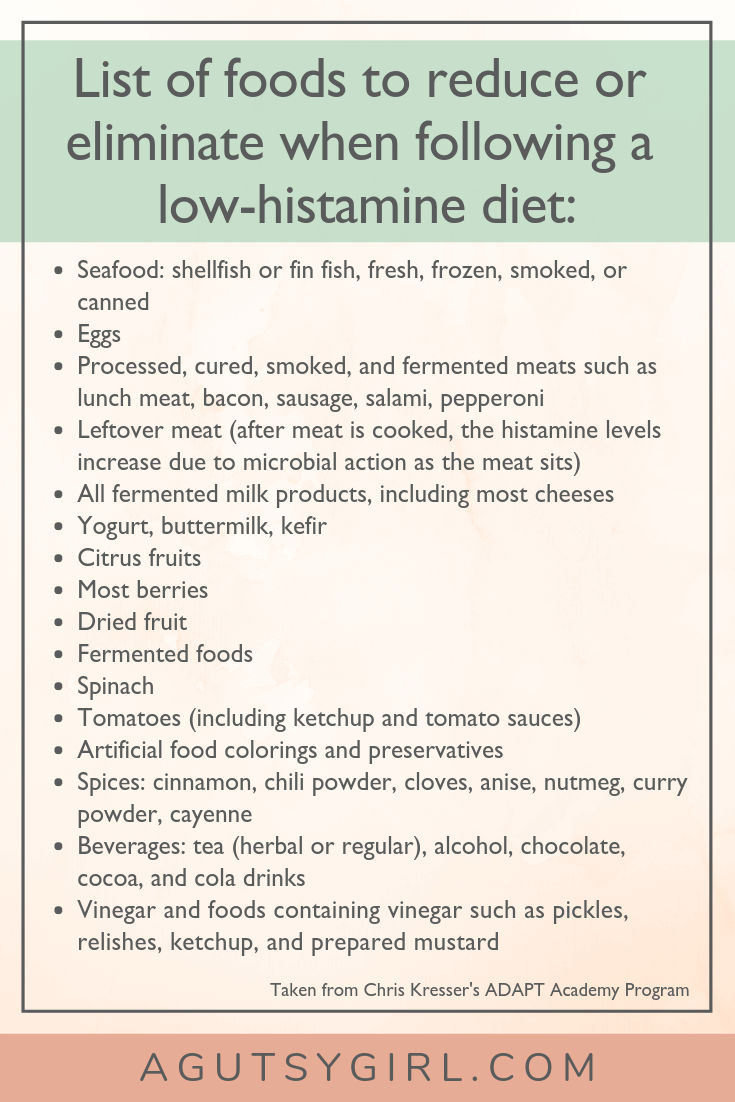

Unfortunately, similar to the Low-FODMAP Diet, many of the foods that contain histamine or provoke histamine production in the body are otherwise healthy foods.
For example, fermented foods, which have extensive benefits, are some of the biggest culprits, since histamine is a byproduct of the fermentation process. (As a side note, Chris mentions that if you have a strong reaction to fermented foods like cheese, wine, kefir, and yogurt, it’s a classic sign of histamine intolerance.)
List of foods to reduce or eliminate when following a low histamine diet:
- Seafood: shellfish or fin fish, fresh, frozen, smoked, or canned
- Eggs
- Processed, cured, smoked, and fermented meats such as lunch meat, bacon, sausage, salami, pepperoni
- Leftover meat (after meat is cooked, the histamine levels increase due to microbial action as the meat sits)
- All fermented milk products, including most cheeses
- Yogurt, buttermilk, kefir
- Citrus fruits
- Most berries
- Dried fruit
- Fermented foods
- Spinach
- Tomatoes (including ketchup and tomato sauces)
- Artificial food colorings and preservatives
- Spices: cinnamon, chili powder, cloves, anise, nutmeg, curry powder, cayenne
- Beverages: tea (herbal or regular), alcohol, chocolate, cocoa, and cola drinks
- Vinegar and foods containing vinegar such as pickles, relishes, ketchup, and prepared mustard
Note: Many probiotics contain histamines, which is why that specific probiotic might not work for you (as a reader commented below). The probiotic I recommend for those with SIBO/histamine intolerance is the Just Thrive probiotic. Learn all about Probiotic Species and Strains HERE.
List of foods to enjoy when following a low-histamine diet:
First and foremost, freshness is key if you have a histamine intolerance. Beyond that, here are some specific foods you can still enjoy:
- Freshly cooked meat or poultry
- Freshly caught fish
- Cooked eggs
- Gluten-free grains: rice, quinoa, corn, millet, amaranth, teff
- Pure peanut butter
- Fresh fruits: mango, pear, watermelon, apple, kiwi, cantaloupe, grapes
- Fresh vegetables (except tomatoes, spinach, avocado, and eggplant)
- Dairy substitutes: coconut milk, rice milk, hemp milk, almond milk
- Cooking oils: olive oil, coconut oil
- Leafy herbs
- Herbal teas
(via Dr. Amy Myers, sourced above)

And guess what? Most people can tolerate histamine foods again once they heal the gut. Ding. Ding. In fact, Dr. Amy Myers says her histamine intolerance was caused by SIBO.
Getting to the root of anything and everything sets you free.
Heal your gut with any of these resources to start today.
- The Leaky Gut Meal Plan: 4 Weeks to Detox and Improve Digestive Health
- FREE 21-Day Gut Healing Inspiration Journey
- Quiz – Where Should I Start on My Gut Healing Journey?
Xox,
SKH


You will heal. I will help.







I’ve had bad allergies all of my life, though they’ve certainly gotten better as I started to eat healither. However, I recently started a probiotic and my allergies went crazy (possibly the worst I’ve ever had). After some research I learned that some strains produce histamine inside the body. My symptoms subsided once I stopped taking that probiotic and now I’m going to be looking for one that doesn’t contain L. buchneri, L. helveticus, L. hilgardii or S. thermophilus (source: https://www.healthline.com/nutrition/probiotics-side-effects#section3). Just thought I would share in case others have had similar issues!
I’ve had bad allergies all of my life, though they’ve certainly gotten better as I started to eat healither. However, I recently started a probiotic and my allergies went crazy (possibly the worst I’ve ever had). After some research I learned that some strains produce histamine inside the body. My symptoms subsided once I stopped taking that probiotic and now I’m going to be looking for one that doesn’t contain L. buchneri, L. helveticus, L. hilgardii or S. thermophilus (source: https://www.healthline.com/nutrition/probiotics-side-effects#section3). Just thought I would share in case others have had similar issues!
Thanks for weighing in!
Eggs are listed in both foods to enjoy and foods to eliminate.
Can you please explain if eggs are ok?
Thank you,
Gretchen
In my research, I did find it on both lists 🙂
M Y brother and I have incurable neuroendocrine cancer ( NET). High histamines in blood. 5-hiaa and we NET patients can not have any histamine high trigger foods which cause our tumors to grow,
Dear Sarah,
As me and both my kids need a low histamine diet, I am used to our cooking needs … when I was reading your list I found some important foods missing on the list you have to avoid!!
If you are sensitive to histamine you must not eat any legumes (including soya!), and any nuts (strawberries are nuts, too, but almonds are nut)! This makes vegetarian/vegan ideals very difficult!
Most HIT-people have problems with pork, beef and poultry is much better.
Wheat is not the main problem, but industrial yeast, so selfmade bread or good(!) old fashioned bakeries are an option.
I hope I can help some people with this information, as the journey of living with HIT can be rough …
Thanks for sharing!
Peanuts are very high histamine, as are the majority of nuts and seeds!