Ever heard of Matula Tea? Certainly you’ve heard about H. Pylori.
What is H. Pylori
Click HERE to save this post for later.
H. pylori bacteria is a common bacteria in the digestive system that attacks the stomach lining.
According to the CDC,
The prevalence of Helicobacter pylori infection worldwide is approximately 50% (1), as high as 80%–90% in developing countries, and ≈35%–40% in the United States.
H. pylori infections are generally innocuous. However, they cause most stomach and intestinal ulcers.
- The “H” stands for Helicobacter.
- “Helico” means spiral, which indicates that the bacteria are spiral in shape.
An H.pylori infection commonly affects children. While this bacteria usually causes no symptoms, it can cause peptic ulcers and gastritis, an inflammation of the stomach.
H. pylori thrives in the stomach’s harsh, acidic environment.
These bacteria can lower the gastric acid of their surroundings so they are able to thrive.
The spiral form of H. pylori permits it to pass through the stomach lining, covered by mucus, and immune cells cannot reach it.
The germs can thwart the immune response, preventing their destruction.
Are you seeing? H. pylori is not a pleasant condition by any stretch of the imagination.

H. Pylori Causes
So what causes H. pylori?
The answer is still somewhat of a mystery.
For thousands of years, humans and bacteria have coexisted. However, the infections are suspected to be spread by mouth-to-mouth contact. They can transmit from a person’s stool to their lips.
In other words, reason 8 million why you must be diligent with your hand washing skills. If you don’t wash your hands correctly after using the restroom, H. pylori can occur.
It also spreads through contaminated food or water.
….but what actually happens?
Once you have H. pylori, the bacteria create stomach issues by penetrating the mucous lining and producing chemicals that neutralize stomach acids.
This exposes stomach cells to solid acids.
Together, stomach acid and H. pylori can create ulcers in the stomach or duodenum, the first segment of the small intestine.
Want a simple breakdown of your digestive system? Click HERE.
What are the symptoms of H. pylori infection?
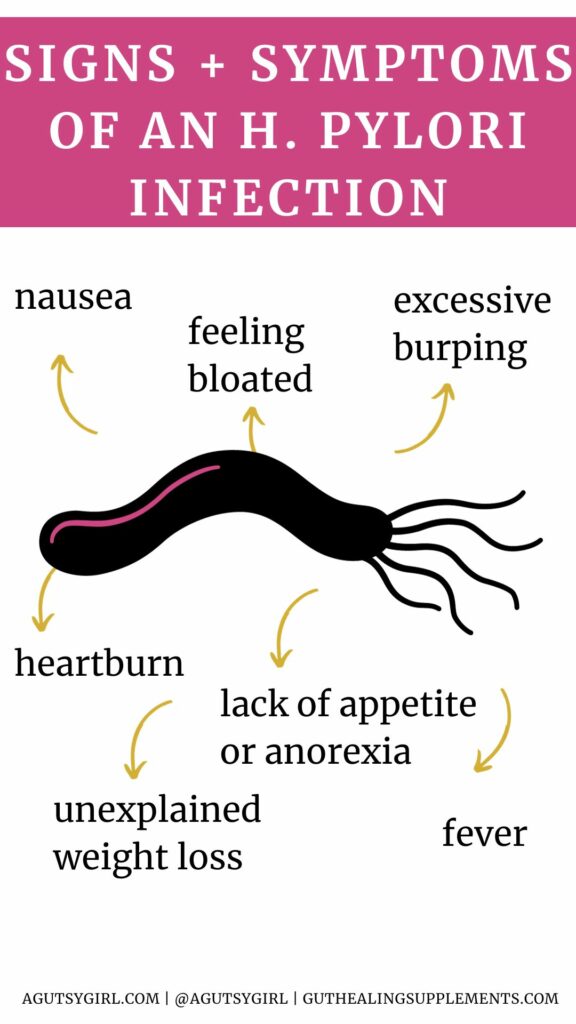
Most H. pylori patients have no h. pylori symptoms, at least not in the beginning.
Symptoms of an ulcer include abdominal pain, especially at night or after meals. The gnawing pain may come and go.
Eating or using antacids may help, which is a strong indicator that a more serious problem could be looming.
If you experience this type of pain that won’t go away, see your doctor.
Make sure you’ve been keeping meticulous track in your gut healing journal, and bring it to your appointment for proof. Want to print your own journal instead of having the printed, spiral-bound copy? Get the instant PDF journal download HERE.
Other signs of H. pylori infection include:
- Excessive burping
- Feeling bloated
- Nausea
- Heartburn
- Fever
- Lack of appetite, or anorexia
- Unexplained weight loss
However, and as always, signs and symptoms overlap with many issues.
The above signs are also frequently in other illnesses as well. In fact, even “healthy” people also experience some H. pylori symptoms.
If any of these symptoms persist or cause concern, visit your doctor.
Who is at risk for H. pylori infection?
Children are more susceptible to H. pylori. Their danger is increase due to poor cleanliness.
Your risk for infection partly depends on your environment and living conditions. Your risk is higher if you:
- Live in a developing country
- Share housing with others who have H. pylori
- Live in overcrowded housing
- Have no access to hot water, which can help to keep areas clean and free from bacteria
- Are of non-Hispanic Black or Mexican American decent
- Too LITTLE stomach acid (see below)
- Long-term use of non-steroidal anti-inflammatories (NSAIDs)
Too LITTLE Stomach Acid
Now, this is something many don’t talk about, but especially for the Gutsy community, I think it’s very important that I do.
H. pylori is always associated with too much stomach acid.
However, many (dare I say most??) actually have too little stomach acid.
The common scenario is this:
- You go into your doctor after a long time dealing with stomach pain, gas, bloating, and a feeling of “fullness” after meals.
- Your doctor says, “I suspect Reflux. Let’s put you on (insert any stomach acid reducing agent) to see if that helps.”
- …..but you get worse.
The reason many times? It was never too much stomach acid to begin with. Many of those symptoms you have could also be due to too little stomach acid. And now do you see what just happened?
Right, you just reduced the amount of stomach acid even more.
This also creates the perfect storm for H. pylori.
If you think this might be you, here are a couple more articles you might benefit from:
- What is Achlorhydria
- How to Test At Home for Low Stomach Acid HCL Challenge
- 33 Ways to Tell if You Have Low Stomach Acid
How are H. pylori infections diagnosed?
Your doctor will inquire about your health and family history. Inform your doctor about all prescriptions, including vitamins and supplements.
If you have peptic ulcer symptoms, your doctor may likely ask about your use of NSAIDs like ibuprofen.
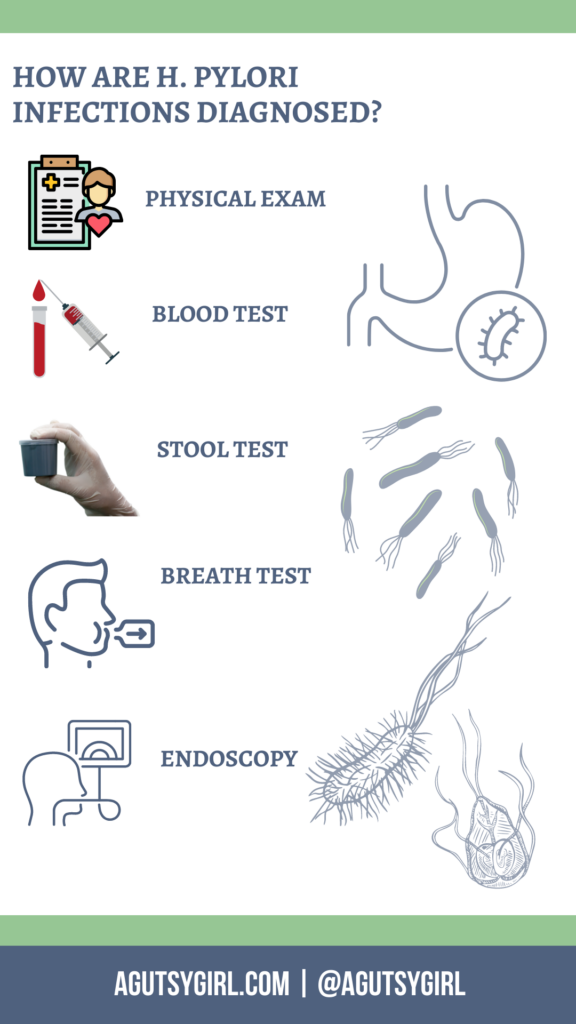
Your doctor may also perform many other tests and procedures to help confirm their diagnosis:
Physical exam
An abdominal exam will look for bloating, tenderness, and pain. They’ll also listen for abdominal sounds.
Blood test
You may be asked to provide blood samples, which will be used to test for antibodies against H. pylori. A healthcare provider will extract a tiny amount of blood from your arm or hand to perform a blood test.
Following that, the blood will be submitted to a laboratory for testing. This is only useful if you have never been treated for H. pylori in the past.
Stool test
It may be necessary to obtain a stool sample to look for evidence of H. pylori in your stools.
Your doctor will provide you with a container to go home with you to collect and store a sample of your feces for future reference. As soon as you return the container to your healthcare provider, they will have the piece sent to a laboratory for further testing and analysis.
These tests and the breath tests would typically need you to cease taking drugs such as antibiotics and proton pump inhibitors (PPIs) before doing the test, but your doctor will notify of you with those changes.
Breath test
Yes, there is also an H. pylori breath test. If this is the route you choose, you will drink a urea-containing solution. H. pylori produces an enzyme called urease, which breaks urea down into ammonia and carbon dioxide.
When the breath test is completed, the goal is for the testing to detect this breakdown and thus provide the diagnosis.
Endoscopy
You are no stranger to the endoscopy because I’ve written about it in detail.
The endoscopy involves inserting a long, thin instrument called an endoscope into your mouth, stomach, and duodenum. A camera attached to the monitor sends images to your doctor. Your doctor can obtain samples from these regions using an endoscope if required.
H. Pylori Test at Home
Everyone always wants to know if you can test at home for H. pylori.
Check out BioHealth Laboratory for an at-home H. Pylori test.
That said, besides that, the answer is that there isn’t really a great, definitive way to test at home.
You can get some preliminary research via your journal and signs and symptoms checklist.
However, due to the severity which can present itself if not appropriately diagnosed, my best advice is to go to your practitioner and ask for the testing.
How are H. pylori infections treated?
If your H. pylori infection isn’t bothering you and you’re not in danger of stomach cancer, therapy may be unnecessary.
H. pylori infection is linked to stomach cancer, duodenal and stomach ulcers.
Your doctor may advise treatment if you have close relatives with stomach cancer or stomach or duodenal ulcers.
Medicine can heal an ulcer and lower the risk of stomach cancer. This therapy for H. pylori is the “H. Pylori Triple Therapy.”
H. Pylori Triple Therapy
Triple therapy is another name for this treatment because this protocol consists of two antibiotics and a stomach acid-reducing medicine.
Antibiotics perform better when stomach acid is lower.
Here are the medications you may see prescribed:
- Clarithromycin (Biaxin)
- Proton pump inhibitor (PPI; examples HERE)
- Metronidazole (for 7 to 14 days) or Amoxicillin (for 7 to 14 days)
Treatment depends on your medical history and if you have any negative side effects to medications.
More H. Pylori Sources: HERE, HERE, and HERE
What is Matula Tea

There is another option for treatment on the market that is getting quite the buzz.
It’s Matula tea, a natural product fitting in the natural treatments category for H. pylori healing.
Now, I want to be very clear with you on something – I have never, ever, ever in the history of this blog, talked about a tea or anything else like that to help heal any condition.
If you want my honest opinion (which is my SOUL purpose for A Gutsy Girl), I remain a skeptic as I recommend for you, too. This research and post on Matula Tea is not medical advice, but rather my curiosity due to many patients and practitioners tell me it did work for them / their patients.
Having said that…..
What is this herbal, Matula Tea?
Matula tea is a 100% organic, wild herbal tea native to South Africa with potent antibacterial properties.
Matula Herbal Tea is effective at killing off 93% of Helicobacter pylori each and every time that Matula comes into contact with Helicobacter pylori in your digestive system. (source)
Additionally, Matula tea is effective against ulcers, candida, and acid reflux, and stomach cancer, all of which can be caused by the bacterial infection Helicobacter pylori.
Matula tea has also been demonstrated to lower diverticulitis inflammation and ulcerative colitis inflammation.
The South African Matula tea contains the following active ingredients (herbs):
- Oleo Europaea & Oleo Africana (Scientific name) Oleaceae (Family name) Olive (Common name) – leaves of the plant (olive leaf)
- Clycyrrhiza Glabra (Scientific name) Fabacase (Family name) Liquorice (Common Name) – root and leaves of the plant
- Cyclopia Intermedia (Scientific name) Fabacease (Family Name) Honeybush (Common Name) – leaves of the plant
- Aspalathus Liniar (Scientific name) Fabacease (Family Name) Rooi Bos (Common Name) – leaves of the plant
- Psidum Guajave (Scientific name) Myrthaceae (Family Name) Wild Guava (Common Name) – leaves of the plant (guava leaf)
- Syzgium Cordathus (Scientific Name) Myrthaceae (Family Name) Afrrican Water Berry (Common Name) – leaves of the plant
- Tulbachia Violcease – (Scientific name) Alliacease (Family Name) Wild Garlic (Common Name) – the root and rhizome of the plant
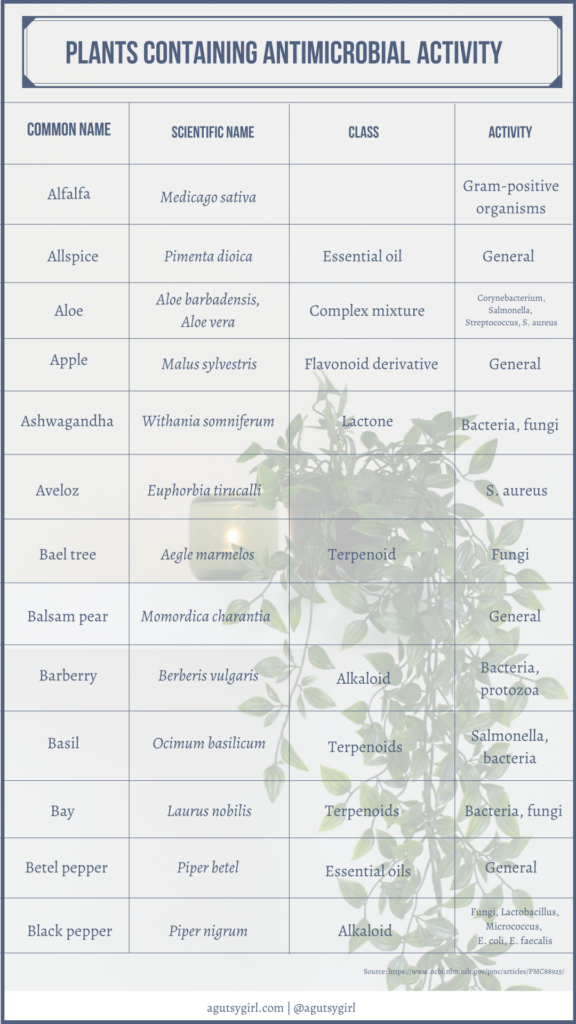
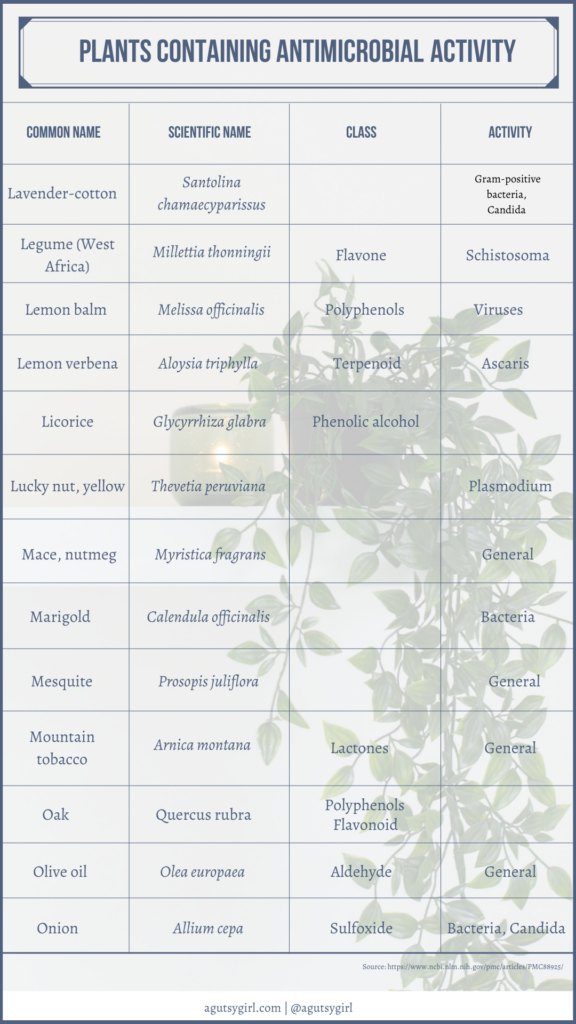
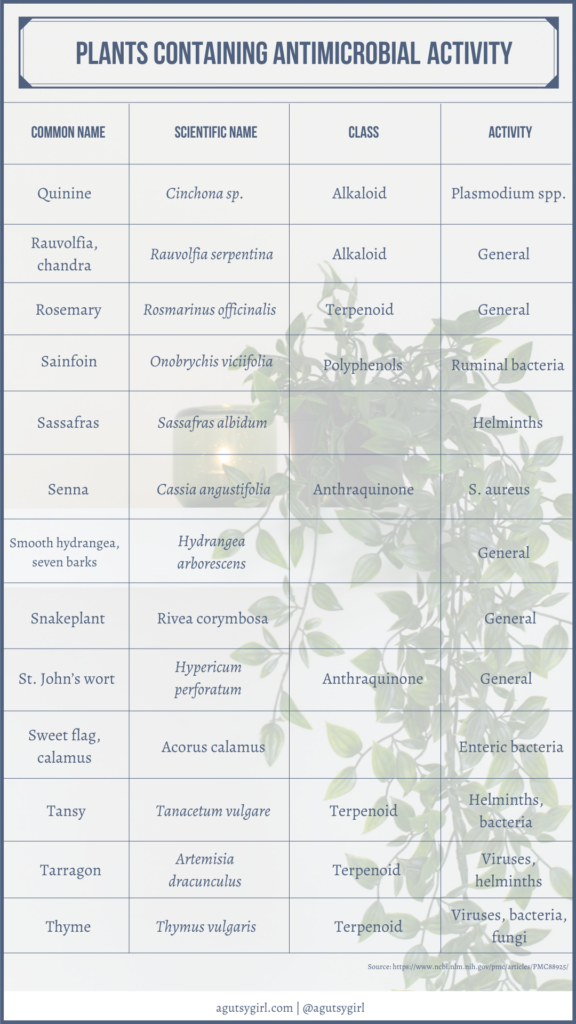
And by the way, using plants as medicine is not some new-age, woo-woo idea.
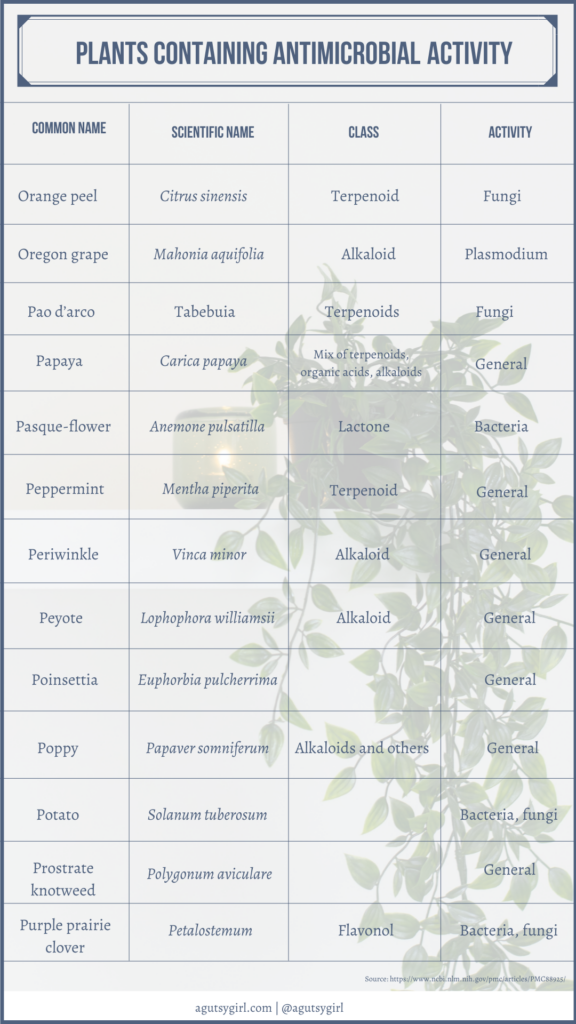
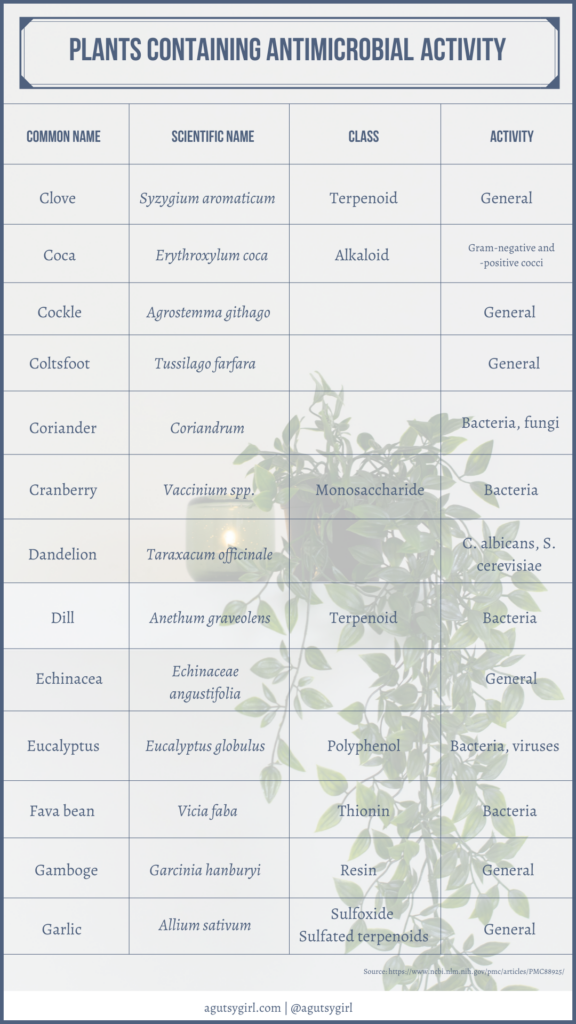
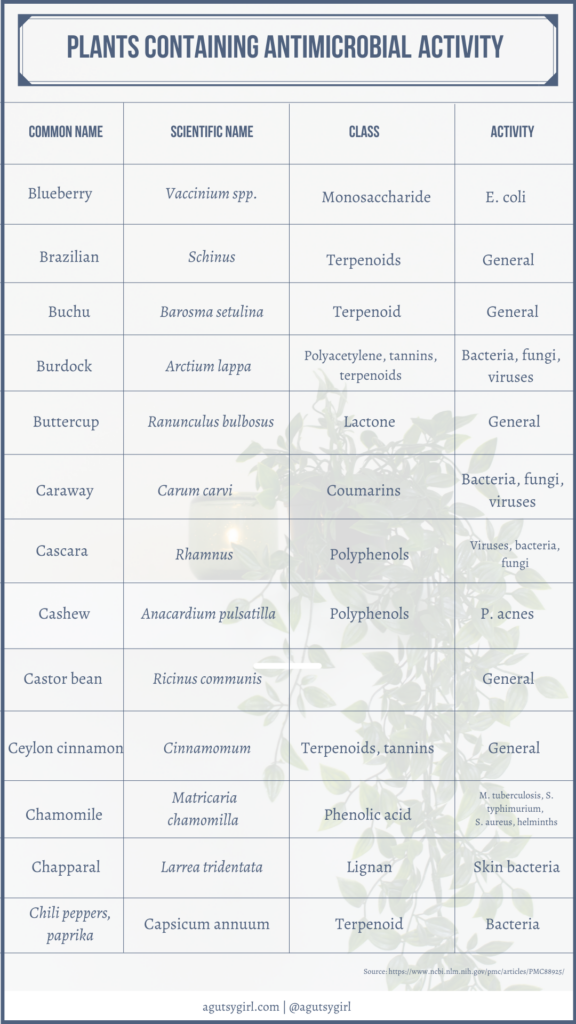
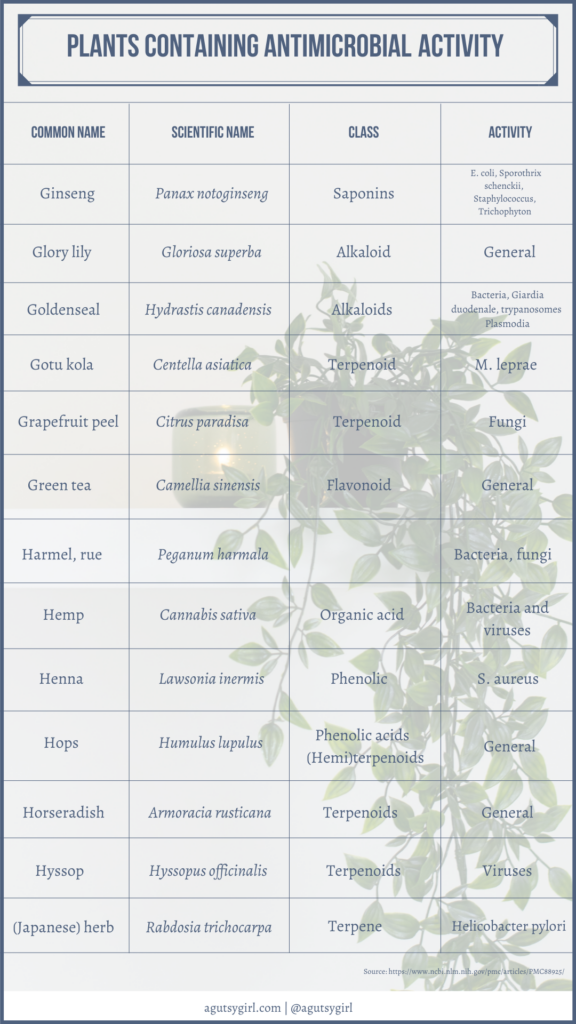
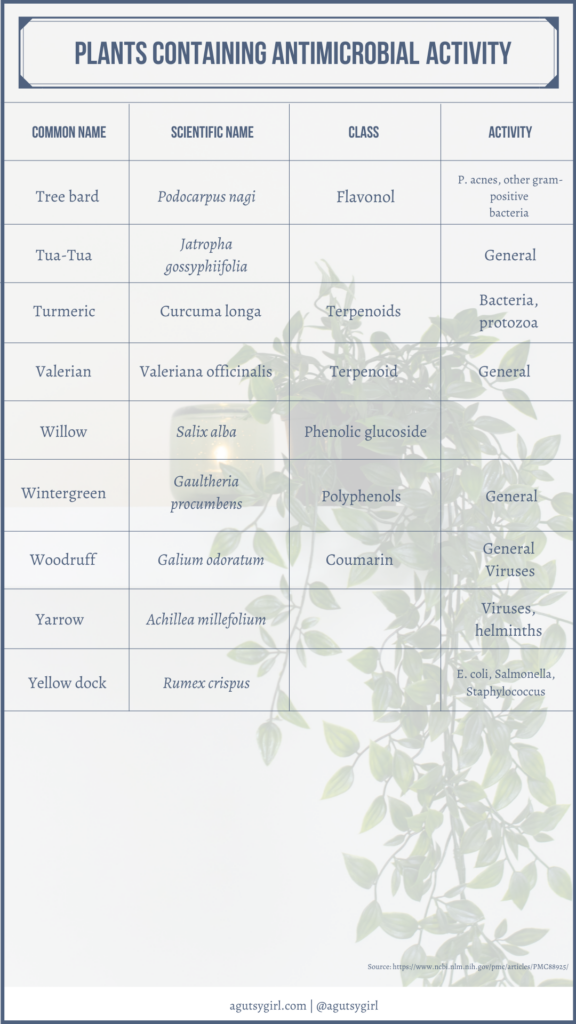
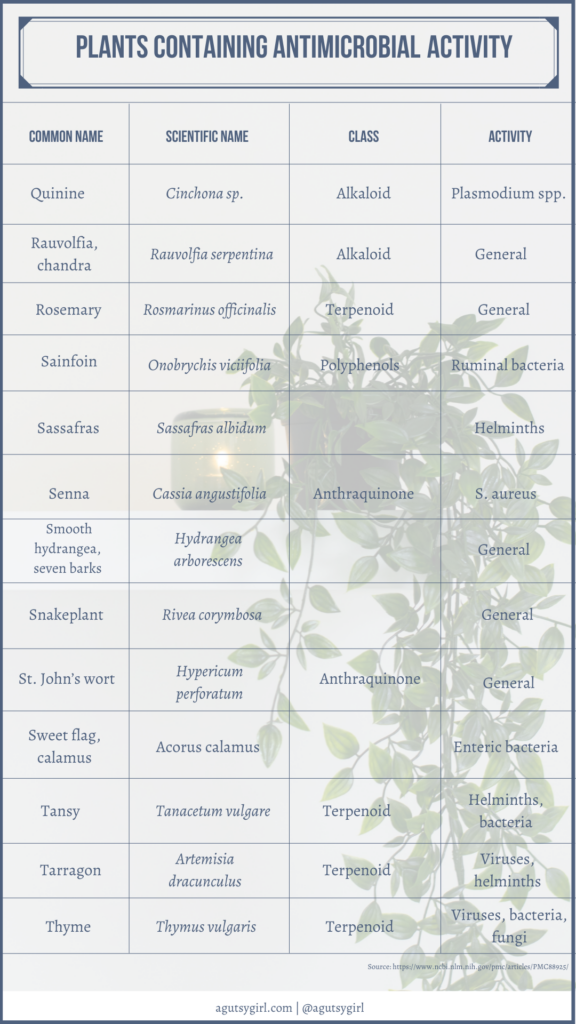
If you want some great reading from a medical journal and the common components of this tea, check out Plant Products as Antimicrobial Agents.
Scroll through to see it all. It’s fascinating!
Matula Tea Benefits
In addition to the above, here are a few more benefits of the effective Matula herbal Tea:
- Long term use is effective against Candida albicans.
- Relieves GERD and Candida symptoms
- Regulates stomach acid production, promoting healing of heartburn and reflux

The Matula Tea Taste
Matula tea is caffeine-free. It’s earthy, like unsweetened green tea.
To make it more palatable, add honey or any other sweetener (although, depending on your condition, do this with caution).
Who should try Matula Tea?
Matula tea has strong indications for people suffering from H. pylori infection as well as for other concerns such as:
- Gall bladder issues
- Loss of appetite
- Burning pain in the stomach
- Nausea
- Vomiting
- Frequent burping
- Loss of appetite
- Bloating
- Diarrhea
- Acid reflux
- Pain in the chest or upper part of the abdomen
- Heartburn
- Unexplained weight loss
- Abdominal cramps
Who is Matula Tea NOT for?
Do not use this tea if you are pregnant or think you might be pregnant. The company also says that even breastfeeding mothers should consult their physician to determine suitability.
Minors should not consume this herbal beverage under the age of 12.
How to make Matula tea?

If you wish to create your own Matula tea formula at home, you can do so by combining the herbs and plants described previously, though doing this is not advised for anyone but an herbalist.
For the rest (99.9% of us!), use the pre-packaged Matula Tea.
According to the Matula Tea website, this is how it works:
- Your Matula Herbal Tea is individually packed in 2 gram (approx. 0.7 ounce) tea sachets and each sachet is sealed in an airtight multi-layer envelope.
- 1 box Matula Herbal Tea comprises 60 tea sachets.
- To make the tea, please place one tea sachet in a tea cup or coffee mug. Pour between 100 and 150 ML (approx. 3.5 to 5 fluid ounces) rapidly boiling, good quality, water over the tea bag.
- Do not add sugar or milk. If desired, half a teaspoon of honey can be added.
- Let the tea draw for at least five minutes.
- Now drink the tea slowly in the morning ½ an hour before breakfast and at night ½ hour before dinner or at least 1 hour after dinner and swirl the tea in the mouth before swallowing.
- Repeat this procedure every day for 30 days- till all the tea has been taken and the treatment course completed.
- You should now feel much better and stomach pains should have disappeared or greatly diminished.
- If pain is still present, then that might indicate that the H Pylori bacteria has not been totally eradicated from your digestive tract.
- In such case, it is imperative to retest for the presence of H.Pylori and this should be done by completing an H.P. Stool Antigen (HPSA) test, not less than 30 days ( max. 45 days) after the completion of the treatment course. Such test can be arranged by your medical practitioner.
Does Matula Tea Work for Getting Rid of H. Pylori?
As I write this article, I am doing an active experiment.
Full disclosure, the company reached out to me to see if I wanted to try it.
I do not have H. pylori nor have I ever had H. pylori. But since so many women in the Gutsy community do, I wanted to explore it for you.
So I said “yes” to researching the product and finding someone who has been diagnosed with H. pylori and was interested in trying the tea.
The tea is currently in her hands, and after her 30 days, I will give a full update.
Matula Tea Reviews
Updated in 2022: Here is the full review and information from Kimberly (from River Falls, WI) who tested it out. Kimberly had all the symptoms in March of 2022, and she had a positive H. Pylori test from a GI Map test.
Update 1: April 13, 2022
She sent me this email on April 13, 2022. At this point, she still had 13 days to go.
Howdy!
Thanks again for allowing me the opportunity to try this.
So, off the bat the directions were a tad confusing. It came with an insert of instructions that said to let the tea draw 10-15 min.
I was all set to do the first morning, and I was going to use it when the actual individual package you open for each tea bag said on it to infuse for 5-10 min. I’m a rule follower with things like this because I want to do it right so I looked for a phone number to call and ask but they just had a website, so I went to check the directions there and it said to it draw at least 5 min 😂 so, I’ve been doing about 10 min.
It does not have that strong of a flavor, I guess just because it’s suppose to be killing h.pylori (and their website says candida and reflux as well) it would be strong.
I am a tea drinker though so I am use to to the flavor, this is comparable to very weak green tea. So, it is pleasant that way for individuals who may not like a strong flavor.
I’ve had no side affects at all. Their website said some people may have gastrointestinal issues.
I’m still having some h.pylori symptoms, burping, etc. I would say it’s the same as when I began.
I have been using it since it arrived 2 xs/day on an empty stomach as suggested.
It can be a little tricky because I’m out the door for work at 6:20 am and this needs to be on an empty stomach (they didn’t say how long you should keep your stomach empty anywhere).
I need to eat so I can leave for work, so I give it about 10 min. on an empty stomach.
At night it’s a little easier because I do have an empty stomach. They say to do it before you go to sleep. But, if I drink before bed I will have to use the bathroom in the middle of the night, that has been happening.
Jury is out if I’d recommend this or doing an herbal h.pylori detox.
Thanks! Hope your day is going well even though it’s been cold and rainy.
Update #2: April 28, 2022
Hi Sarah,
I’m done with the tea. Right after I emailed I had some pretty bad burping and throat feeling a tad raw.
I had to start using my bitters and lemon water that I gave up before trying out the tea to see if that would help by increasing my stomach acid, and it did.
I know h. pylori can cause low stomach acid so I was hoping doing the tea would get rid of that symptom for me but it didn’t.
It’s hard to say if it worked or not as I still have some of my h. pylori symptoms. I see my functional med doctor in a couple weeks and can ask about testing for h. pylori again.
Thanks for the opportunity again and let me know if you have questions about my experience! I’ll be buying your book and plowing through your suggestions soon.
AGG Thoughts: June 22, 2022
I just reached out to her to see if she ever had the chance to retest, which is key in this equation, since the company has an excellent guarantee:
After completion of the Matula Tea treatment, you are covered by our money-back guarantee if:
- You test Positive after completing an H.Pylori Stool Antigen test or
- Your H.Pylori count is greater than 1.0e3 after completion of the GI Map test.
- The HPSA or GI Map Test should only be done 4 weeks (between 30 and maximum 45 days) after completion of the course. The 4 week delay is requested due to the fact that the digestive system needs this period of time to eliminate any dead Helicobacter Pylori bacteria).
The company also makes note:
Please email us a copy of your doctor’s ‘Before and After‘ HPSA test (H. Pylori Stool Antigen test ) or a recent GI-Map stool test, including your order number to support@matulatea.com which should confirm that the Helicobacter Pylori has not been fully eradicated and that you are still infected. Once we have received the signed and dated HPSA test or GI Map test written or typed in English and we will refund you your total purchase price.
The full guarantee verbiage is HERE.
Some other follow-up comments I’ll make:
- I recorded a podcast episode on Gastritis, H. Pylori, and Acid Reflux. You can listen to the episode HERE.
- As you also likely made note, she was not able to follow all instructions to a ‘T.’ However, where she did not, I personally wouldn’t think would make a huge difference, but we can’t be certain on that.
- H. pylori, like SIBO, is super hard to get rid of. And if whatever caused it to begin with is not addressed, I still do not believe there is any strength of a cup of tea, herbal antimicrobial, antibiotic, or anything else that will take care of the problem.
- Reason #4,567 for checking out my course ‘Gut Healing: ELEVATED.’ 🙂
Have more questions? If you personally have tried the tea, I’d LOVE to hear from you! I’d love to verify the company’s proven success rate!
If you liked this post, you might also enjoy:
Xox,
SKH







H.pylori
I used Matula tea, late last year and on retesting had a negative test and all symptoms had subsided. Unfortunately 5 months later the symptoms are back and I seem to have been reinfected.
My family members weren’t keen to be tested last time, but I’m now thinking they should be. I can only think my reinfection is caused by a local sushi shop, the deli counter at my supermarket (both of which I hadn’t eaten from for several weeks; or someone close to me that has H.Pylori.
The Matula tea worked amazingly and I was pain free, but it is very expensive if it needs to be repeated often.
Thanks for all the great thoughts, Karen!
I’m so excited to try Matula Tea! I’ve heard so many great things about it.
I’d love to hear how it works for you 🙂
Have you heard any other success stories about the tea? My daughter tested positive for h pylori so we are giving it a try. I am doing it too .
Hi, Courtney – these are the ones I personally know, but I think there are many on their own website as well 🙂