I was just about to do more research and share all about GI hormones when week 2 of the Gut Health Course popped up with the subject.
In any case, I’m super excited to share this information.
By the way, I have a whole podcast episode with Dr. Pedre all about women’s gut health and hormones. Check in out HERE.
All About GI Hormones
Click HERE to save this post for later.
Now, this information can get fairly technical. In fact, while going through this Gut Health Course, I am part of a private Facebook group for it.
Someone in the group said (with regards to this topic), “It seems sooo complicated. I’m taking it a step at a time and trying to understand the process…slowly.”
Because I don’t want to bore or inundate you with unnecessary things, I’m just going to try to give you the goods today.
What are (GI) Gastrointestinal Hormones?
GI Hormones or Gastrointestinal Hormones are,
chemical messengers that are implicated in many aspects of physiological functions of the gastrointestinal tract, including the regulation of secretion, absorption and digestion, and gut motility. GI hormones are a large family of peptides and are secreted by endocrine cells that are widely distributed throughout the GI mucosa and pancreas.
Did you know that the gut has more endocrine cells than anywhere else in the body? It is also the largest endocrine organ.
Depending on the research, context, and source, you’ll find different GI hormones listed. In fact, did you know that there are more than 50 gut hormones and peptides synthesized and released from the GI tract?
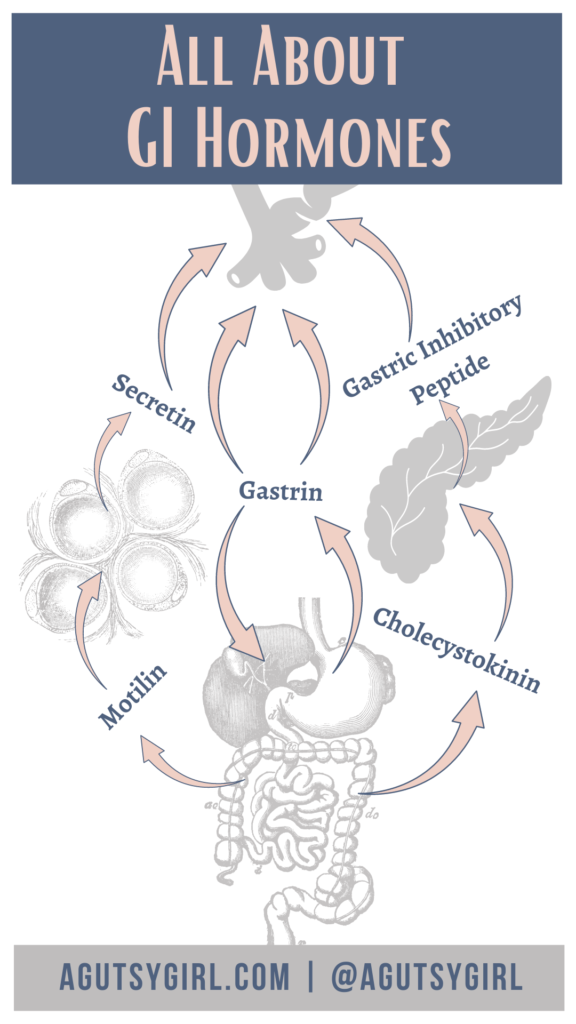
At Nutrition School, we took a look at these five digestion regulating hormones:
- Gastrin
- Secretin
- Cholecystokinin
- Gastric Inhibitory Peptide (GIP):
- Motilin
Gastrin
When it is stretched, the stomach secretes gastrin. Its function is to stimulate the release of hydrochloric acid and pepsin for digestion. It also stimulates stomach lining growth and motility.
Secretin
The duodenum secretes secretin. (Now, say that 10 times in a row!). Its function is to help regulate water and pH. It also stimulates the pancreas to release sodium bicarbonate; the liver to produce bile.
Secretin has the effect of stimulating the pancreas to produce alkaline secretions as well as slowing the emptying of the stomach.
Cholecystokinin
The duodenum also secretes cholecystokinin. And its function is to stimulate the gallbladder to release bile. It also release digestive enzymes in the pancreas when fat is present.
Gastric Inhibitory Peptide
Also known as GIP, Gastric Inhibitory Peptide is secreted from the stomach. Its function is to slow stomach churning and inhibits acid as chyme moves from the stomach to small intestine.
GIP also stimulates insulin secretion, and induces satiety.
Motilin
Motilin is secreted from the duodenum. It increases the migrating myoelectric motor mobility, which is also known as the MMC (migrating motor complex). This role is to “clean” the intestines during a regular fasting period.
I have talked about the benefits and powers of the MMC via Intermittent Fasting and Meal Spacing.
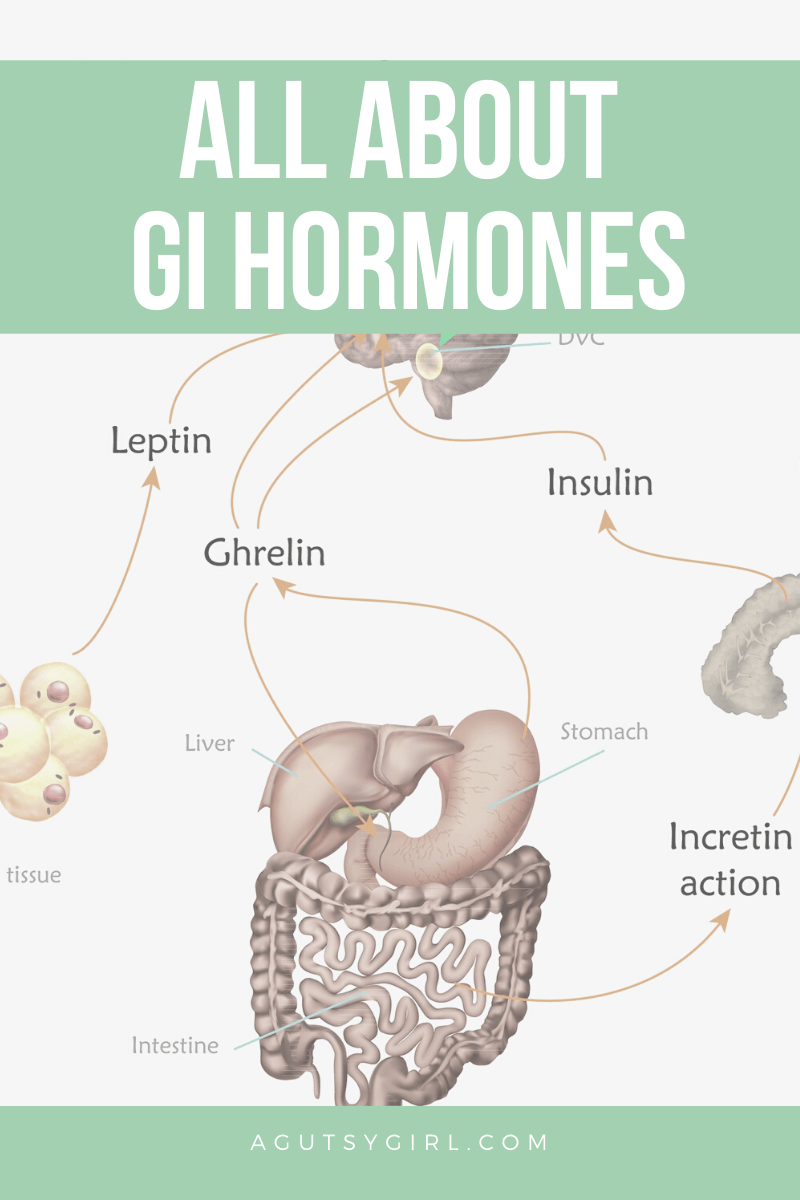
In addition to the five digestion regulating hormones, there are also the two hunger hormones. These include: ghrelin and leptin.
Ghrelin
Your stomach secretes ghrelin. It targets the pituitary gland, signaling an empty stomach.
This hormone increases appetite and tells your body, “I’m hungry. Feed me now, or else.” 🙂
Leptin
On the contrary, fat cells make leptin. It signals fullness and plays a role in decreasing appetite.
To start understanding more about your body, digestion, and hormones, consider using a food and lifestyle journal.
I have one that you can print off in PDF format HERE. Otherwise, I can ship the beautiful, spiral-bound 90-day journal right to your doorsteps.
If you liked this post, you might also enjoy:
Sources: Gut Health Course – IIN, HERE, and HERE.
Xox,
SKH
🤰 bloating be gone! weight loss through optimal gut health for women
💃ʜᴇᴀʟ ʏᴏᴜʀ ɢᴜᴛ. ʜᴇᴀʟ ʏᴏᴜʀ ʟɪfe.
🫶🏻 founder gutbyome.com







Thank you for the overview–your posts are always helpful.